Information on Monkeypox
Since May 13th, 2022, infections of the monkeypox virus have been reported across 12 World Health Organization (WHO) regions. Clusters of this virus were found, though not exclusively, in groups that identified as MSM (men who have sex with men).
As of May 21st, 2022, there have been 92 confirmed infections and 28 suspected cases of monkeypox, some of which have been confirmed in Pittsburgh. A Pittsburgh resident recently went viral on TikTok for discussing her difficulties in receiving a monkeypox diagnosis -- until she visited our team at Central Outreach Wellness Center.
In light of these developments, the team at Central Outreach Wellness Center wants our patients to be informed about the risks, effects, and prevention of monkeypox in order to mitigate its spread, as well as the steps they can take to get tested.
Here are some basic facts about how the virus was discovered:
- The monkeypox virus belongs to the Orthopoxvirus genus
- Monkeypox was first discovered in 1958 when two outbreaks occurred in colonies of monkeys kept for research and was later disseminated by rodents
- The first human case of monkeypox was reported in the Democratic Republic of the Congo in 1970
Infection with monkeypox occurs:
- After contact with an animal, human, or materials contaminated with the virus
- When the virus enters through broken skin, respiratory tract, or mucus membranes in the eyes, nose, and mouth
- Through human-to-human transmission, which usually happens through large respiratory droplets
- Through exposure to bodily fluids, lesions, or materials that have also been exposed (like bedsheets, clothing, etc.)
Keep reading to learn more about the monkeypox virus, monkeypox signs and symptoms, risk factors for monkeypox, preventative measures, and what to do if you think you may have been infected. If you have questions, don’t hesitate to reach out to us.
If you have active lesions, contact us today and get tested!
855-5-WE-CARE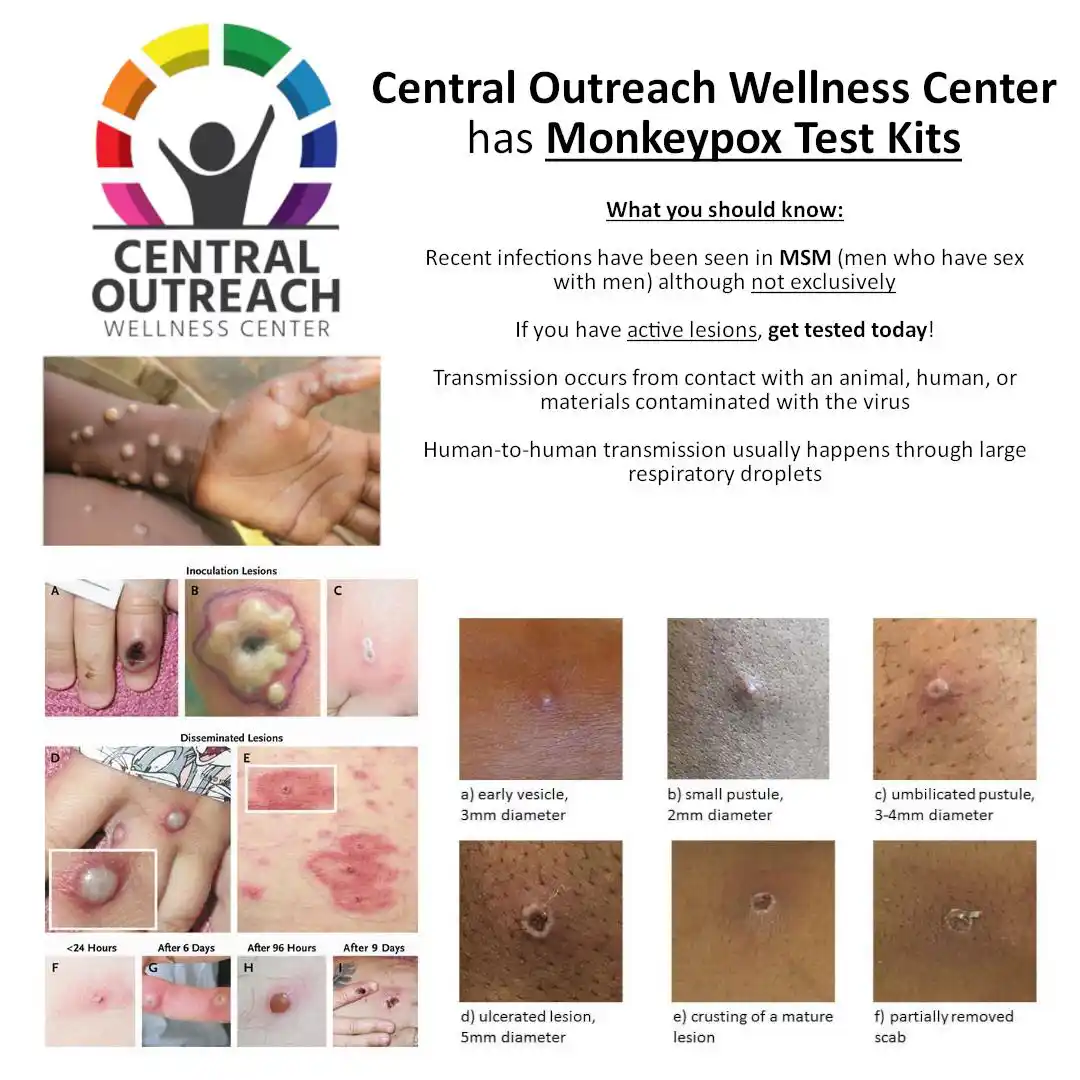
What is Monkeypox?
Monkeypox appears similarly to ordinary discrete smallpox – it’s characterized by lesions that progress over time into pustules and then scabs. However, monkeypox will also feature swelling in the lymph nodes.
The incubation period of monkeypox can last 7-14 days, during which a patient is not contagious and may feel fine. Following this period, the progression of the virus is as follows:
- Prodromal period: First signs appear, including fever, malaise, headache, weakness, and sometimes sore throat and cough. The lymph nodes may swell in the neck (submandibular & cervical), armpits (axillary), or groin (inguinal) and can occur on both sides of the body or just one.
- Rash: Lesions will develop in the mouth and on the body. These lesions go through several stages and are considered contagious through scabbing.
Once lesions appear, they may progress as follows:
- Macules (1-2 days): A macular rash appears on the skin, starting on the face and spreading.
- Papules (1-2 days): Lesions have progressed to macular (flat) and papular (raised).
- Vesicles (1-2 days): Lesions become raised and filled with fluid.
- Pustules (5-7 days): Lesions become filled with opaque fluid, sharply raised, usually round, and firm to the touch.
- Scabs (7-14 days): Pustules have crusted and scabbed over before falling off.
When properly administered before exposure, existing smallpox vaccines are effective at protecting people against monkeypox. There are three currently licensed vaccines in the United States to prevent smallpox, which will be released by the CDC as needed for confirmed cases or exposure:
- ACAM2000: Administered as a live virus preparation that is inoculated into the skin by pricking the skin surface. Following a successful inoculation, a lesion will develop at the site of the vaccination. The virus growing at the site of this inoculation lesion can be spread to other parts of the body or even to other people, so individuals who receive vaccination with ACAM2000 must take precautions to prevent the spread of the vaccine virus.
- JYNNEOSTM: Administered as a live virus that is non-replicating. It is administered as two subcutaneous injections four weeks apart. There is no visible “take” and as a result, no risk for spread to other parts of the body or other people. People who receive JYNNEOS TM are not considered vaccinated until they receive both doses of the vaccine.
- Tecovirimat (ST-246): Central Outreach has partnered with the CDC and now is able to offer TPOXX(tecovirimat) for clients with presumed ocular risk, penile lesions, or peri-anal lesions. Studies indicate effectiveness in treating orthopoxvirus-induced disease.
While not much data is available on alternate treatment options for monkeypox in humans, several options are being researched for potential use:
- Cidofovir and Brincidofovir (CMX001): Data unavailable in humans. Both have been proven effective in vitro and in animal studies.
- Vaccinia Immune Globulin (VIG): data is not available for treatment of monkeypox complications. VIG can be considered for prophylactic use in an exposed person.
Frequently Asked Questions
What are the guidelines for suspected monkeypox?
The WHO guidelines state that monkeypox may be suspected in a person of any age presenting in a monkeypox non-endemic country with an unexplained acute rash who is also displaying one or more of the following signs or symptoms, since 15 March 2022:
- Headache
- Acute onset of fever (>38.5oC),
- Lymphadenopathy (swollen lymph nodes)
- Myalgia (muscle and body aches)
- Back pain
- Asthenia (profound weakness)
Additionally, the clinical picture must not be explained by the following common causes of acute rash:
- Varicella zoster
- Herpes zoster
- Measles
- Zika
- Dengue
- Chikungunya
- Herpes simplex
- Bacterial skin infections
- Disseminated gonococcus infection
- Primary or secondary syphilis
- Chancroid
- Lymphogranuloma venereum
- Granuloma inguinale
- Molluscum contagiosum
- Allergic reaction (e.g., to plants)
- Any other locally relevant common causes of papular or vesicular rash
If I suspect I may have been exposed to monkeypox, what should I do?
The CDC has created a Monkeypox Exposure Questionnaire in response to the 2022 Monkeypox outbreak to assist in assessing patient exposures prior to illness onset. It contains seven sections, four of which can be adapted to fit specific situational needs.
View the questionnaire here(opens in a new tab), and if you do qualify for suspected exposure, reach out to your provider at Central Outreach as soon as possible for the next steps.
Where can I read more about monkeypox from reliable sources?
WHO:
CDC:

